Location
Primary Location
2950 College Dr. Suite 2H
Vineland, NJ 08360 US
-
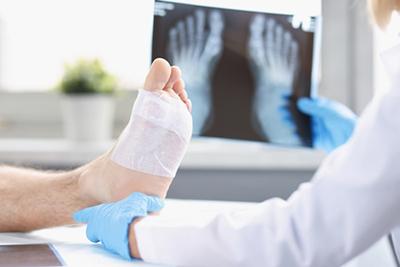
The Role of Podiatry in Managing Foot and Ankle Fractures
posted: Feb. 14, 2024.

-
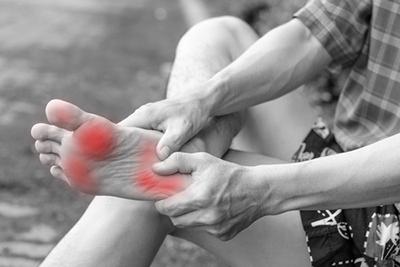
Common Foot Problems: Identifying and Addressing Ailments From Heel to Toe
posted: Feb. 12, 2024.
-
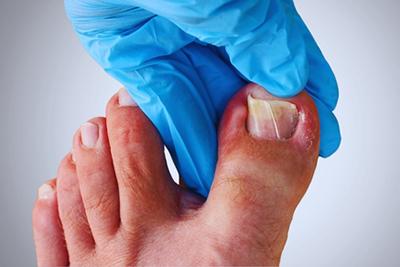
What You Need To Know About Ingrown Toenails
posted: Feb. 01, 2024.
-
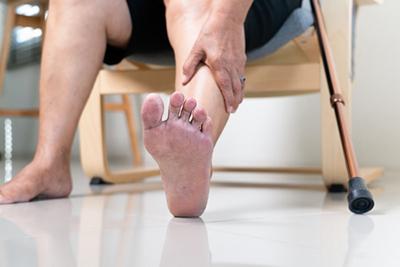
Sports Podiatry: Addressing Foot and Ankle Injuries in Athletes
posted: Jan. 08, 2024.

-
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
posted: Jan. 01, 2024.

-
Diabetic Foot Care: Preventing Complications and Maintaining Foot Health
posted: Dec. 07, 2023.
-
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
posted: Dec. 01, 2023.

-
The Benefits of Seeing a Podiatrist
posted: Nov. 07, 2023.

-
Causes of Heel Pain
posted: Nov. 03, 2023.
-
The Benefits Of Orthotics
posted: Nov. 01, 2023.

-
When To See a Podiatrist
posted: Oct. 06, 2023.

-
The Importance of Diabetic Care
posted: Oct. 01, 2023.

-
Treating Your Bunion Symptoms
posted: Sep. 14, 2023.

-
Bunion Treatment Options
posted: Sep. 01, 2023.

-
When You Should See a Podiatrist for Ankle Pain
posted: Aug. 09, 2023.
-
Foot Health for Children
posted: Aug. 01, 2023.


